New Public Course Dates Announced for 2018
We have published our Paediatric First Aid courses for April 2018 to March 2019. We have included Saturday, weekday and evening courses. In addition we have added a Blended Learning courses in Whictchurch and Worcester.
Also, we are holding a Buccal Midazolam course on the 12 February and Level 2 Safe Handling and Administration of Medication course on the 13 February at our training rooms here in Worcester.
For more information please contact Craig on 01905 745457 or craig@cognet.training
Robin Walker MP Visits Cognet
Cogne
Cognet Chosen as CIEH Premium Centre
Cognet can confirm that we have been chosen by the Chartered Institute of Environmental Health to participate in the CIEH Premium Centre scheme.

Cognet Wins Prestigious Environmental Health Award

(L-R) Tim Everett, President of the CIEH, David Fortnam, Nick Gregory, Paul Stedman, Stuart Fellows, Andy Statham, Chair of CIEH’s Board of Trustees
Paul Stedman and Stuart Fellows of Bridgnorth and Worcester were recently presented with a prestigious award having been recognised for their services to field of environmental health.
The awards ceremony was organised by the Chartered Institute of Environmental Health (CIEH), a leading professional membership body that works in the public, private and non-profit sectors to raise environmental health standards through training and guidance.
The event took place on Tuesday 14 July 2015 at the House of Lords and were sponsored by Lord Rooker PC, former Chairman of the Food Standards Agency.
The awards recognised people who have excelled in the field of environmental health, in areas such as food safety, housing standards and public health, and were presented to both professional Environmental Health Officers and members of the public who work in the field.
Paul and Stuart received the Best Training Centre Award for achieving the highest student mark in the Level 4 Award in Managing Food Safety in Catering and demonstrating consistent quality standards in training delivery and centre administration.
Paul Stedman said: “We were honoured to receive such a prestigious award. Professionals working in the field of environmental health often fly under the radar so it’s nice to know that the CIEH truly values the contribution we make to local communities, their health and wellbeing.
“We would also like to thank and congratulate our colleague Nick Gregory for achieving the Trainer of the Year Award and to David Fortnam, of Aston Villa Football Club for achieving Student of The Year for his highest score in the Level 4 Award.”
Chief Executive of the CIEH, Graham Jukes OBE, said: “These yearly awards provide the opportunity for the CIEH to recognise and celebrate those who have gone above and beyond the call of duty. All the winners today have delivered excellent environmental health services, using their skill, passion and dedication, making positive examples for all of us to follow.
“More importantly, it is the hard work of these people that directly contributes to the health and wellbeing of the average person on the street.”
On the day, awards were presented by Tim Everett, President of the CIEH, Andy Statham, Chair of CIEH’s Board of Trustees and Lieutenant Colonel Geoff Ward, Chair of CIEH Ltd Board.
Cognet Awarded CIEH Best Centre Award for 2014

Cognet have been a registered training Centre with the Chartered Institute of Environmental Health for 8 years and in that time we have run 650 CIEH courses from Level 1 Introductory courses to Level 4 Management courses.
Cognet will strive to maintain it’s high standards of delivery and management of all our courses ensuring continued high levels of customer and learner satisfaction.
Treatment of an Acute Asthma Attack

Asthma attacks may be triggered by a variety of different irritants, such as pollens, animal fur, house dust mites, exercise or infection. The muscles around the walls of the airways tighten, so that the airways become narrower. The lining of the airways become inflamed and swell, and there may be increased production of mucus or phlegm which can plug the airways, narrowing them further.
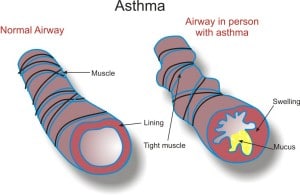
Treatment of asthma is aimed at two goals: relieving symptoms and preventing future symptoms and attacks. Often a daily (preventer) inhaler is used to control inflammation. In the event of an attack a ‘reliever’ inhaler helps to manage the symptoms. The most common reliever inhaler is salbutamol (Ventolin ™) and is blue. People with asthma should have a personal action plan, agreed with their GP or asthma nurse that includes information about the medicines they need to take, how to recognise when symptoms are getting worse, and what steps to take when they do so.
SIGNS AND SYMPTOMS
Coughing at rest
Wheezing sound from the chest at rest
Difficulty breathing, possibly with use of muscles in shoulders and upper body to help.
Chest tightness
More serious symptoms include:
Unable to talk, or to complete a full sentence
Exhaustion
Blue/white tinge around lips
Collapse
If these symptoms are present, call 999.
TREATMENT OF AN ACUTE ASTHMA ATTACK
Remain calm and reassuring
Encourage the patient to stand or sit upright, or leaning slightly forward, relax their shoulders and concentrate on breathing out
Help the patient to take their inhaler correctly. Children, particularly younger children, should use a spacer. Two puffs of inhaler through the spacer may be given every two minutes up to a maximum of ten puffs if required. If the child does not feel better at this stage, or if you are worried earlier, call 999.
If an ambulance has not arrived 10 minutes after the initial 10 puffs have been completed, and the child is still unwell, repeat the process.
If treatment is successful, and the patient feels better, they may resume normal activities.
Head Injury Guidance
Minor head injuries, or bumps to the head, are common in children. If there has been no loss of consciousness, and there is no deep cut or severe damage to the head it is unusual for there to be any damage to the brain. Rarely, though, there may be bleeding within the skull which causes pressure on the brain, symptoms of which may take hours, or even days, to occur. Carers should be alert to these signs as they may indicate a serious condition needing urgent treatment.
WHEN TO CALL 999 OR SEEK IMMEDIATE HELP
If there has been any loss of consciousness
Fall from a height (> 3 metres) or high speed injury (road traffic accident, hit by projectile)
Blood or clear fluid leaking from ears or nose
Abnormal drowsiness or behaviour, confusion or problems understanding or speaking, or in nonverbal children inconsolable or inconsistently consolable crying
Seizure
Weakness in part of body, dizziness, loss of balance or uncoordinated movement
Problems with vision, such as blurred or double vision
More than one episode of vomiting
Headache which is not resolved with paracetamol, or which gets steadily worse
Inability to remember events leading up to or after the injury
WHEN TO SEEK LESS URGENT ADVICE (e.g. GP, minor injury or walk in centre)
If none of the above signs are present but
Fallen from a height greater than the child’s own height or greater than one metre
Fallen downstairs
Suspicion of deliberate harm (abuse)
Under one year old
Vomiting (but see above re more than one episode)
Known blood clotting disorder
Has consumed alcohol
WHEN IT IS APPROPRIATE TO KEEP WATCH AT HOME
If none of the above signs are present and
If there was no loss of consciousness
Minor bruising or grazing only
Cried immediately, but can be consoled and otherwise interacts normally

Observe the child for 2-3 days, or until symptoms have settled, if you become concerned about their behaviour or responses seek further advice. Encourage them to get plenty of rest and avoid strenuous activity. Pass on information about the event to other care-givers so that they can also observe the child.
WOUND CARE
Minor wounds can be cleaned with tap water. Bumps and swellings can be treated by applying a cold facecloth.
Larger cuts may need further treatment, but in the first instance stop the bleeding by applying pressure over the wound, using a sterile wound dressing or clean cloth.
Braun Thermoscan IRT3020 Tympanic (in-ear) Thermometer
The latest Tympanic (In ear) Thermometer from Braun
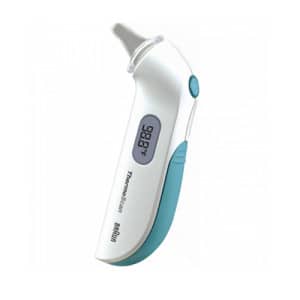
This thermometer is suitable for all the family. Its compact design is easy to use. It measures and displays a temperature in just one second. It measures the heat generated within the ear, and provides very accurate, professional level results while being quick, easy and gentle, minimising disturbance for your child.
LCD display shows readings in Celsius and Fahrenheit.
Its Memory function recalls the last temperature reading.
Auto shut off after 60 seconds.
Lens filters reduce the risk of transferring germs.
Lens filters from previous models are compatible.
Latex-free
Braun is the number one brand with doctors and healthcare professionals
Price £29.95 (includes VAT) Plus £2.99 P&p
![]()
Guidance on Fever in Children

An increase in temperature in itself is not dangerous, and can often be treated at home. Fevers in children are not uncommon, and sometimes even after full examination there may be no reason found for a fever.
LOOKING AFTER A FEVERISH CHILD
Give the child plenty of drinks, such as water or squash. Give babies smaller but more frequent feeds. If you are breastfeeding then continue to do so.
Do not worry about food if the child does not feel like eating, but encourage them to drink more.
Signs of dehydration include dry mouth, lack of tears, sunken eyes or producing less urine. In babies, the soft spot on the head (fontanelle) may be sunken. If you notice any of these signs, seek further advice from your doctor or via 111.
Do not over- or under-dress a child with fever. Physical methods of cooling a child, such as fanning, sponging with tepid water etc are not advised.
It is not necessary to use medication to treat fever, but if the child is distressed paracetamol or ibuprofen can help them to feel better. Always follow the instructions on the bottle.
Check on your child regularly, including during the night, especially infants.
WHEN AND WHERE TO SEEK HELP
If the child
Becomes unresponsive
Struggles to breathe or becomes blue
Has a fit
Develops a rash that does not disappear if a glass is pressed firmly against it
CALL 999 OR GO STRAIGHT TO YOUR NEAREST ACCIDENT OR EMERGENCY DEPARTMENT.
Contact your GP or NHS111 if
The child’s health gets worse or you are worried
If the child develops signs of dehydration (dry mouth, no tears, sunken eyes, sunken fontanelle, reduced output of urine), is drowsy and seems generally unwell
A high temperature lasts more than 5 days and the child has not yet seen a health professional
If the child is less than 6 months old
